Do you, or your loved one, have a painful arthritic knee? Perhaps they haven’t been to a specialist yet, but their GP has acknowledged that their knee pain is due to arthritis? Well whether their need for a knee replacement has been confirmed by an orthopaedic surgeon or not. Here is everything you need to know about knee replacements.
When is a knee replacement required?
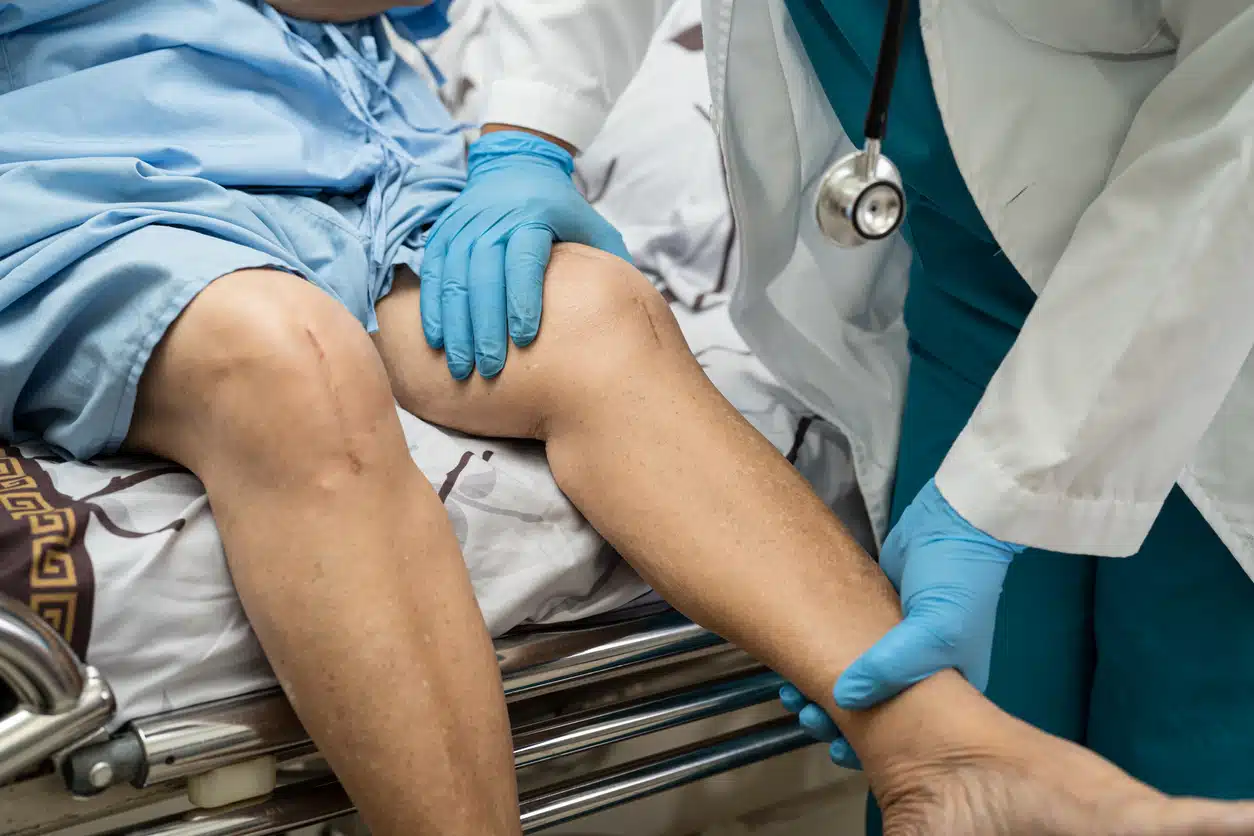
Specialists only recommend total knee replacements when the patient has an extremely painful and badly worn knee, which is normally due to arthritis. If the pain in their knee is affecting their everyday life and they’ve tried physio, then it’s time to get a referral from their GP to see a specialist. The source of their knee pain will be investigated and if the source is arthritis and their knee has degraded enough, a total knee replacement is the only option. Specialists take knee replacements very seriously and try to avoid giving them to people under the age of 50.
Benefits of a knee replacement
Replacing the arthritic knee with an artificial joint will allow pain-free walking and activities of daily life! A knee replacement provides the patient with many years of quality life and relief from pain.
Implications of a knee replacement
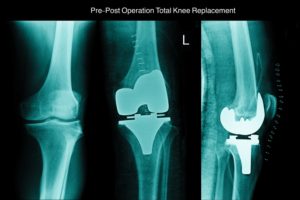
An artificial knee will never function in exactly the same manner as the original knee. The artificial knee is made of metal (chrome cobalt or titanium) and a plastic (high-density polyethylene) joint bearing that will slowly wear over the years. If too much wear occurs, the knee may become loose and painful or the components may even break!
It is important for patients to treat their knee carefully and avoid excessive activities that may shorten the life of the artificial joint. High-impact activities such as running, tennis and aerobics should be avoided.
Walking for exercise, the use of an exercise bicycle and swimming are excellent forms of exercise that are not detrimental to your artificial knee.
Artificial knees require regular “check-ups”. 6months after the surgery the patient should be seen, then every year thereafter following the operation. For each yearly visit, an x-ray of the knee will need to be performed beforehand so it can be taken to the check-up.
Before the knee replacement
- The patient will be admitted to hospital on the morning of surgery.
- The patient should expect to be in the hospital for five days.
- No anti-inflammatory drugs can be taken at least five days prior to surgery. This is because the drugs, Voltaren, Nurofen, Brufen, Feldene, and Indocid (Celebrex is not a problem) can increase the risk of bleeding. However, if the patient is on low-dose aspirin (eg. to prevent stroke or heart attack) they may continue to take those.
- The skin near the operation site must be kept clean. If you have a cut or a pimple in the knee area, the surgeon needs to be notified prior to surgery.
Hospital admission
- The patient cannot eat or drink 6 hours prior to surgery admission. This is because the operation list order can change unexpectedly.
- Want to bring:
- Consent Form
- Personal items (comfortable pyjamas, slippers, dressing gown, toiletries)
- Any current medication
- All relevant x-rays, scans and reports
- Prior to going into surgery, the patient will:
- Be dressed in a theatre gown and disposable underwear
- Have special stockings fitted (to help prevent blood clots)
- Be asked to mark the painful leg with an arrow on the thigh using a marker.
After the knee replacement
-
The same day:
- Directly after the surgery, the surgeon can speak with a family member in person or on the phone.
- The patient will be returned to the ward, where they will be resting in bed.
- They will have a drip in their arm for fluids.
- They will have a bulky dressing over the wound on their knee and special stockings on their legs designed to help reduce the risk of blood clots forming.
-
The day after:
- The blood count will be checked and an x-ray of the appropriate knee performed.
- Under the guidance of the physiotherapist, the patient will be stood up and usually takes a few steps.
- The patient will start taking a single aspirin tablet a day (300mg) with food. This will be continued for six weeks and is designed to help thin the b
lood slightly and prevent blood clots in the legs or elsewhere.
-
A couple days after:
- The physiotherapist will take the patient for a walk and give them instructions about theiractivities during the recovery period, including an exercise programme.
- For pain control, the patient will have injections (Morphine) and tablets (Panadeine Forte) available. Most people require either no injections or only one or two, as tablets are usually enough to control the pain.
-
By day five most patients are ready to go home.
Recovery at home – what to expect
- By the time the patient returns home, they should be able to safely get into and out of beds and chairs and go up and down stairs. However, some patients may require changes to their housing, such as ramps or rails or aids in the bathroom. These requirements should be discussed with the doctor prior to the surgery so that appropriate arrangements can be made timely.
- Whilst waiting for their strength and mobility to return, patients may need help with meals, bathing and being comfortable. If the patient is returning home on their own (and don’t have family support) then interim help can be arranged.
- Some pain in the operated knee is expected (not as severe as the pain was before surgery). It will gradually decrease in the first few weeks.
- Patients can take the tablets given to them as needed for pain.
- 12 days after the surgery the dressings should be taken off. If it falls off before this and the wound is clean, that is fine.
- There are usually no stitches to remove (as they are dissolvable). There is sometimes a mild reaction (redness and inflammation) around the wound when the stitches are dissolving.
- The wound should be kept clean and dry until the wound is completely healed (12 days). Waterproof covering for the shower. No baths or pool swims where the wound is submerged.
- Stockings should be worn for six weeks.
- The patient should follow the physical activity and exercise guidelines given to them by their physiotherapist.
- The first four weeks should be spent resting at home. The level of activity should then slowly increase with an aim to be back to most activities at six weeks.
- The patient should be safe to drive at six weeks following their first postoperative review by their orthopaedic surgeon. They will be reviewed by Dr Sterling six weeks after surgery.
Dr Sterling should immediately be contacted if:
- The wound becomes hot, red or swollen or begins to ooze fluid
- Severe and constant pain in the knee or leg develops
- There is bleeding or discharge from the wound
- The patient is unwell and has a fever
- The patient has chest pain or shortness of breath
- There is increased swelling in either leg or pain in the calf
Hopefully, this article answers most, if not all your preliminary questions about total knee replacements. If you do think of any queries, please don’t hesitate to contact us at Greg Sterling Orthopaedics.